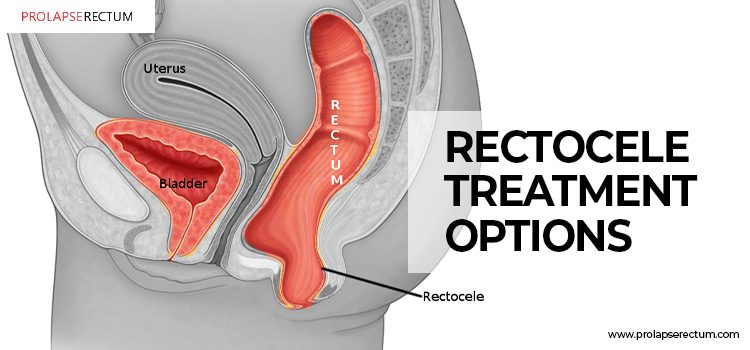
In women, a strong wall of thick, fibrous tissue called fascia separates the vagina from the rectum. When a section of this wall becomes weak, a portion of the rectum bulges into the vagina. Rectocele is the medical term for this protrusion.
When the wall is damaged during vaginal birth, the issue frequently arises. After a vaginal birth, the bulge may appear, although symptoms may not appear until later in life. Rectoceles are more frequent in women over the age of 50 who have reached menopause.
Persistent constipation, chronic cough, recurrent heavy lifting, or any action that causes pressure on the pelvic floor over time may all raise the chance of developing rectocele.
Because minor rectoceles often generate no symptoms, it’s difficult for doctors to say how frequently they occur. Rectoceles may afflict as few as 20% of adult women or as many as 80%, although they are most frequent in elderly women who have had repeated vaginal births. The average rectoceles patient in a recent study of 125 women in the United States was about 60 years old, in menopause, and had had two or three vaginal births. A woman with a rectocele is more likely to develop a cystocele (an abnormal bulging of the bladder caused by a weakening in the anterior vaginal wall) and uterine prolapse (abnormal sagging of the uterus into the vagina because of loss of its pelvic support).
Treatment
If you have rectocele symptoms, your doctor will most likely perform surgery to restore the weakening in the tissue connecting your rectum and vagina. This repair may be as simple as using stitches to reinforce the region, or it can be as sophisticated as using a mesh patch to strengthen and maintain the wall between the rectum and the vagina. If you also have a cystocele or uterine prolapse, these diseases may typically be treated at the same time as your rectocele repair.
As an alternative, a vaginal pessary, a noninvasive therapy, is offered. A pessary is a ring-shaped, block-shaped, or plug-shaped device that is inserted into the vaginal canal to support the bulging tissues. There are many varieties of pessaries in use, some of which you may be able to remove and clean on a daily basis, and others that may need a doctor’s visit for removal and cleaning on a regular basis. Your doctor will choose the optimum sort of pessary for you and ensure that it fits appropriately.